From Student to Patient: How Keck Medicine of USC Brought Me Back to Life
USC’s Post-COVID clinic guided this USC alumna on her journey back to health
At 30 years old, I sat coloring in bed. It was all I could do.
Deep blues, daffodil yellows and emerald greens filled the ink-stained outlines in my coloring book. I strained to stay in the lines as my world spun on a perpetual leftward tilt. It was early February 2021 in North Carolina, and I had been sick with long COVID-19 for nearly three months. I was deteriorating fast: I’d lost 20 pounds, I barely slept, I had severe and constant vertigo, and I could only speak in a slow, drunk-like drawl.
Life looked vastly different from when I graduated from the USC Annenberg School for Communication and Journalism and the USC Dornsife College of Letters, Arts and Sciences with a double bachelor’s degree in journalism and political science at the top of my class in May 2020. Back then, I was on the fast track to a dream career in journalism—one that I’d gone back to school for in my mid-20s to pursue as a first-generation transfer student.
Now it took all the mental energy I could muster to simply color inside the lines.
The adult coloring book—a very adult coloring book, featuring flowery curse words—arrived two days before, along with a box of colored pencils and a handwritten letter from Christina Bellantoni, my former journalism professor and mentor at Annenberg. Bellantoni was one of three people outside my family who knew what was happening to me. A smile crept across my face from time to time as I colored in offensive words that summed up how I felt about this illness.
“Coloring is supposed to be good for brain healing,” she had written. “I was told that USC is starting a post-COVID clinic. We can try to get you in.”
The idea of USC’s post-COVID clinic offered me and my family something we had scarcely dared to feel that winter: hope. We let that sliver of hope buoy us from the cold and sterile North Carolina exam rooms of “I don’t know” toward the possible spaces of “I can help.”
Two weeks later, my husband, Jerry, drove us across the country in an SUV newly purchased for the trip. Jerry pulled out of the suburban North Carolina neighborhood and went across the expansive bridges of the Mississippi River, the flatlands of West Texas, the red-dirt canyons of southeast New Mexico, and then, finally, the palms, dry heat and gridlock of Southern California.
A couple of weeks later, I was accepted as a patient at what would become the COVID Recovery Clinic at Keck Medicine of USC.
‘Long COVID seems to be a thing’
Dr. Caitlin McAuley recalls that early in the COVID-19 pandemic—around June 2020—she began seeing patients who weren’t getting better after COVID infections had ended.
“People were starting to acknowledge, ‘Hey, long COVID seems to be a thing,’” says McAuley, a physician and clinical assistant professor of family medicine at the Keck School of Medicine of USC. “It seems to be more complicated—something we need to have a specialty clinic for.”
In response, Keck Medicine set up a post-COVID outpatient clinic in December 2020 to treat and study the unusual symptoms that can follow a COVID infection. Jehni Robinson, chair of the Department of Family Medicine at the School of Medicine, appointed McAuley to oversee it and treat patients. The outpatient clinic was the precursor to the launch of the COVID Recovery Clinic, which officially opened in 2022.
Keck Medicine set up a post-COVID outpatient clinic in December 2020 to treat and study the unusual symptoms that can follow a COVID infection.
“The funny thing is, at first, the Family Medicine department put a general email for participation in the clinic out, and I think a lot of Keck staff were hesitant because it was something new, and we weren’t used to it,” McAuley says. But while most doctors shied away from diving into a new post-viral illness because of its unfamiliarity and workload, McAuley leaned into the challenge.
Operated through two of Keck’s departments, pulmonology and primary care, the clinic is located at Keck’s medical campus in East Los Angeles. There, McAuley sees COVID patients once a week.
The clinic offers a targeted approach to symptom management through referral. Its staff of six— a family medicine physician, physical therapist, social worker, respiratory therapist, pulmonologist and nurse—evaluates patients before sending them to various Keck specialists.
Patient demand and the waitlist for the clinic have ebbed and flowed with surges in COVID cases, which tend to spike about a month after cases rise. Its approach to treatment also evolves as doctors learn more about the illness’s impact on patients’ lives and livelihoods. The clinic now offers an anti-inflammatory diet protocol–eating foods known the reduce inflammation in the body such as tomatoes, leafy greens, berries and fish, and avoiding sugar, bread, pasta and fried food. A social worker also informs patients at appointments about potential disability programs and other social service options available to them.

McAuley says she’s noticed patterns: Some symptoms cluster together. Loss of taste and smell, for example, tend to go with neurological symptoms such as cognitive dysfunction, chronic headaches, insomnia, dizziness and sensory issues. Respiratory symptoms, such as prolonged cough, shortness of breath and severe fatigue, are present in some patients. Some patients present three or four of these “clusters,” she says.
She’s seen some patients’ symptoms improve after getting a COVID-19 vaccine, and some studies have shown antihistamines can also be helpful. But there are no proven treatments for long COVID yet. As with most medical research, that will take time and money.
Good on paper
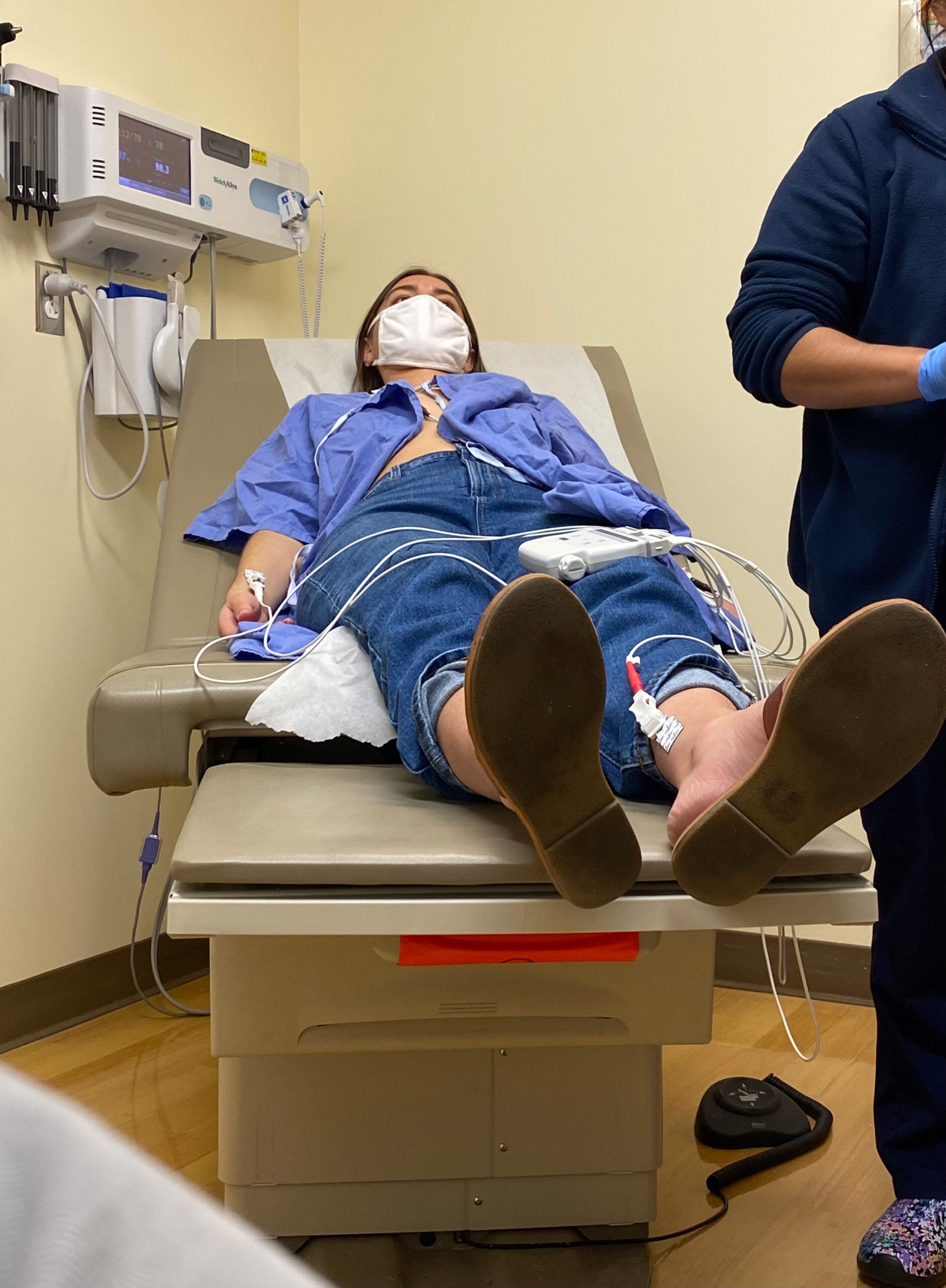
In April 2021, I signed in for my first appointment at the clinic. My nurse Cindy Ho and I walked back and forth through the hallway while a machine and pulse oximeter measured my vitals.
One foot in front of the other, I pushed forward. My muscles were tired and achy, and I craved to lay down, but the oximeter showed nothing out of the ordinary. For the nth time, I was withering away and yet told I looked “good” on paper. Then I met with McAuley. She asked plenty of probing questions striving to understand my experience and symptoms.
I was withering away and yet told I looked “good” on paper.
Morgan Stephens
Next was a meeting with a social worker. I was impressed that the clinic understood that long-haulers were in dire straits. Many are too sick to work and see doctors constantly—a recipe for financial ruin in the United States.
Since my symptoms were primarily neurological, the clinic referred me to a neurologist, an occupational therapist and a physical therapist. Finally, we had a plan to tackle my illness from various specialists to get me functional again.
Ashley Halle, an associate professor of clinical occupational therapy at USC Mrs. T.H. Chan Division of Occupational Science and Occupational Therapy, worked with me on pacing and rest.
Since the pandemic started, Halle has seen a steady flow of long COVID patients. Demand is cyclical, depending on the latest surge in cases. Her work focuses on meeting patients’ needs and goals to get them back to being functional. Her department has seen dozens of long COVID patients. Symptoms, she says, include fatigue, mental health symptoms like depression, anxiety, suicidality and cognitive symptoms like brain fog and concentration problems.
“It’s really about partnering with them, [noting] where they are right now in their lives, and where they want to see themselves in the future,” Halle says, “then coming up with a plan on how we can get them to that place of wellness, recovery, and their new normal.”
Planning for life with long COVID
Healing from long COVID looks different for everyone.
I knew I was getting better when my world widened beyond surviving each day to planning for life—an actual life—with long COVID.

I started earning victories with small tasks like pouring my own coffee, making a meal, or taking a short walk. Some patients return to their pre-COVID selves, while others can become disabled for months—with gradations in between.
As I worked with the Keck clinic team, our focus turned to ensure that I would be OK when resting. The agitation and anxiety accompanying my neurological symptoms made me feel as if I was always in “fight or flight” mode.
“Let’s call them ‘brain breaks,’” Halle said during one of our sessions. This meant no phones or computers, no problem-solving and no tasks, so my brain would have 10 minutes to simply rest.
Halle and I met over Zoom to discuss my capacity, triggers and pacing. We started tracking my migraines on an app.
After a month of working together, I told her that we’d accumulated enough small victories that I was ready to go for a big win: I would try going back to work at CNN. I was terrified, but I needed to see what I was cognitively and physically capable of. I quickly found that five days a week was too exhausting—plus, I needed time for my doctor’s appointments. I sometimes had multiple appointments a week with different specialists.
But I was able to work again. A year after being treated, I felt good enough to close my long COVID chapter. I started seeing my doctors less, eventually stopping my weekly appointments. I’d made it to the other side. Nearly two years after graduating, I’d achieved another rite of passage through USC.
Helping other long-haulers
Today, I’m back in North Carolina. The stifling silence and sadness I once associated with the place have given way to laughter, long walks in nature, full nights of sleep, and work after a nearly two-year hiatus. We’re looking to buy a house in Washington, D.C., a city I love and initially dreamed of working in after I graduated.
McAuley wants the COVID Recovery Clinic to serve as a model that can help other long-haulers like me.
“I hope we can work on education and spread this toward our primary care population because it will be hard for everyone to get into these kinds of clinics,” said McAuley. “As we learn more and better therapies, people can go to their regular doctors for [long COVID].”
When people ask how I got better, I realize there’s no one answer: Many factors combined into that big push back to the land of the living. But I know that my alma mater took me in as a shadow of who I was and walked with me as I slowly stitched myself back together, piece by piece, treatment by treatment, until I resembled myself again.
That’s more than what a “medical center” does. It’s what a family does.
