New Alzheimer’s treatments won’t be widely accessible without changes to national health systems
USC research shows how several major countries could prepare their health systems to ensure patients can get Alzheimer’s treatments once they hit the market.
The first disease-modifying Alzheimer’s treatments are on the horizon, but health systems in the United States and Europe would have to take a number of steps to ensure they are ready to provide those treatments to the millions of people who need them, according to two USC reports presented this week at the Alzheimer’s Association International Conference.
Soeren Mattke — a research professor of economics at the Center for Economic and Social Research (CESR) at the USC Dornsife College of Letters, Arts and Sciences — assessed the hurdles to providing these treatments to people with Alzheimer’s disease in the United States, as well as in France, Germany, Italy, Spain and the United Kingdom.

“As the COVID-19 pandemic has taught us, even the most sophisticated health care systems can be overwhelmed by sudden surges in the demand for services,” Mattke wrote. “The arrival of a disease-modifying treatment for Alzheimer’s disease may result in a similar scenario, in which current health system capacity is insufficient to cope with the expected influx of patients who will seek diagnosis and treatment.”
He and co-author Mo Wang, a research assistant at USC Dornsife, found that the countries have various gaps in their health care systems that, if unaddressed, make it difficult for many patients to access treatments once they have been approved for use. Mattke, a physician and health services researcher who directs the CESR Center for Improving Chronic Disease Care, focused on problems in the countries’ health care systems, as well as in their capacity and their capabilities to deliver treatment.
While these countries’ systems differ in many ways, they have some problems in common, including a lack of funding for memory testing that would help identify people who have Alzheimer’s disease and, with the exception of Germany, a shortage of specialists trained in cognitive testing.
Necessary health system changes regarding Alzheimer’s include funding, technology
Mattke gathered the information for the reports by conducting 30 expert interviews and examining multiple databases, research published in peer-reviewed journals and technical reports.
Some of the health system barriers likely to impede access to treatment include:
- Funding: While all countries have or are in the process of developing national dementia strategies, none have devoted funding to implement the recommendations. Further, several diagnostic tests that are part of the patient journey are not fully covered by health systems. It is assumed, but by no means guaranteed, that the approval of a treatment would lead to coverage of the necessary tests.
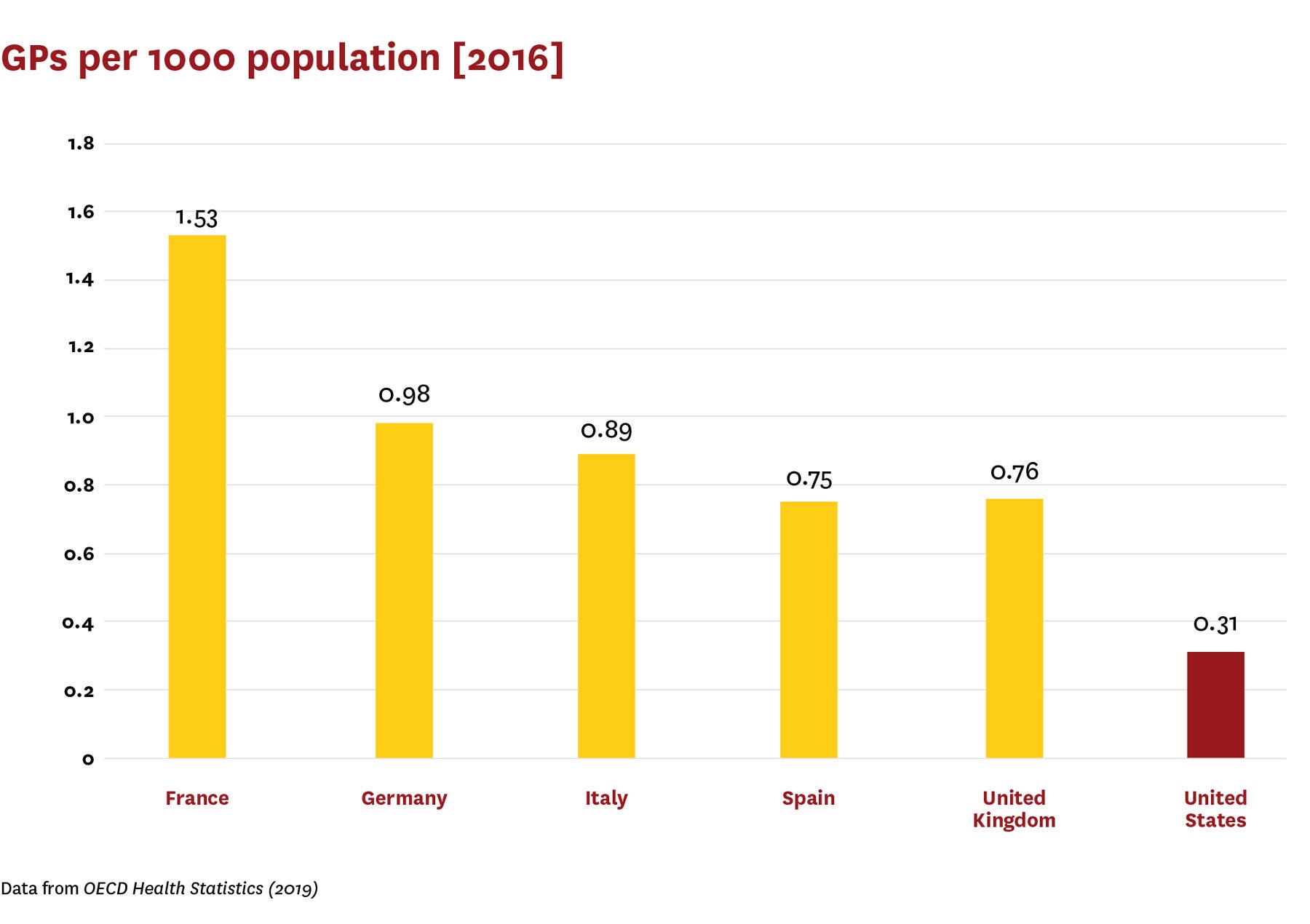
- Workforce: Primary care physicians in all countries remain reluctant to assess cognitive function because of incompatibility with their workflows, lack of training and tools, and a perceived lack of therapeutic consequences. Dementia specialists are in short supply in all countries, leading to lengthy wait times in the diagnostic process. The United States has 8.8 such specialists per 100,000 people, and France has the fewest in the group with 6.5 per 100,000. While Germany leads the pack with 24 specialists per 100,000 people, incentives are lacking for those clinicians to increase patient volume.
- Technology: Countries have limited capacity to conduct PET brain scans to diagnose Alzheimer’s disease. Not even the United States — with five PET scanners per 1 million people — would have sufficient capacity, and many patients in rural areas would face geographic obstacles. Countries like France, Germany and Spain only have about two scanners per 1 million people, and the U.K. only has 0.5.
While these findings point to a need to devote additional resources to memory care, engage primary care physicians in case finding and triage, and leverage scarce dementia specialists’ time more effectively, there are encouraging initiatives in all six countries.
A simple blood test for Alzheimer’s disease could become available soon, which would greatly improve the diagnostic process. diagnostics. France has set up a national network of memory clinics for routine care and for research. Germany introduced an annual comprehensive geriatric assessment including cognitive decline. Italy launched a program, the Interceptor Project, to track patients with early-stage Alzheimer’s disease with the objective that doctors could identify patients at risk of faster progression. In Spain, an expert group formed a group to conduct regional assessments of system readiness for memory care and provide recommendations. The U.K. initiated an accreditation scheme to standardize memory services. In the U.S., Project ECHO is experimenting with telehealth models to empower primary care clinicians to provide memory care.
“Alzheimer’s disease poses a unique challenge because so many different clinicians and planners must work together to prepare for the advent of a disease-modifying treatment,” Mattke said. “A concerted effort of stakeholders will be needed to raise awareness for this challenge and work on solutions. Unlike in the COVID-19 pandemic, there is still time for health care systems to prepare. But the work needs to start now.”
The work was funded by a contract from Roche, known as Genentech in the United States, a company that is developing blood-based assays and disease-modifying treatments for Alzheimer’s disease, to the University of Southern California. The sponsor had no role in the design of the study, interpretation of the findings or decision to submit the data for presentation at AAIC.



